Affordable homes for key workers: addressing the particular pressures in Health and Social Care
Data Insights
Published by
PriceHubble
-
17 Feb 2026

Affordable homes for key workers: addressing the particular pressures in Health and Social Care
Data Insights
Published by
PriceHubble
-
17 Feb 2026

Affordable homes for key workers: addressing the particular pressures in Health and Social Care
Data Insights
Published by
PriceHubble
-
17 Feb 2026

At the end of January, PriceHubble partnered with the Association for Rental Living (ARL) to host a discussion on a challenge that sits at the intersection of housing markets and public services: how the lack of affordable homes impacts the lives of key workers, particularly those employed in Health and Social Care.
The webinar brought together three complementary perspectives – market data, academic research, and delivery expertise – to explore what is now widely recognised as more than simply a housing problem.
Chaired by Sandra Jones, Managing Director at PriceHubble UK, the panel featured Dr Iqbal Hamiduddin, Associate Professor at UCL’s Bartlett School of Planning, Sarah Hordern, Non-Executive Director at the Oxford University Hospitals NHS Foundation Trust, CEO of Perspicio and Chair of the NHS Homes Alliance, and Julia Middleton, Real Estate Economist at PriceHubble.
Together, their contributions painted a consistent picture: housing affordability is critical to staff recruitment, retention and wellbeing.
The scale of rental dependence among healthcare workers
To set the scene, Julia Middleton shared metrics from PriceHubble’s achieved rents and renter demographics dataset, offering insights into the scale and characteristics of healthcare workers living in the private rental sector.
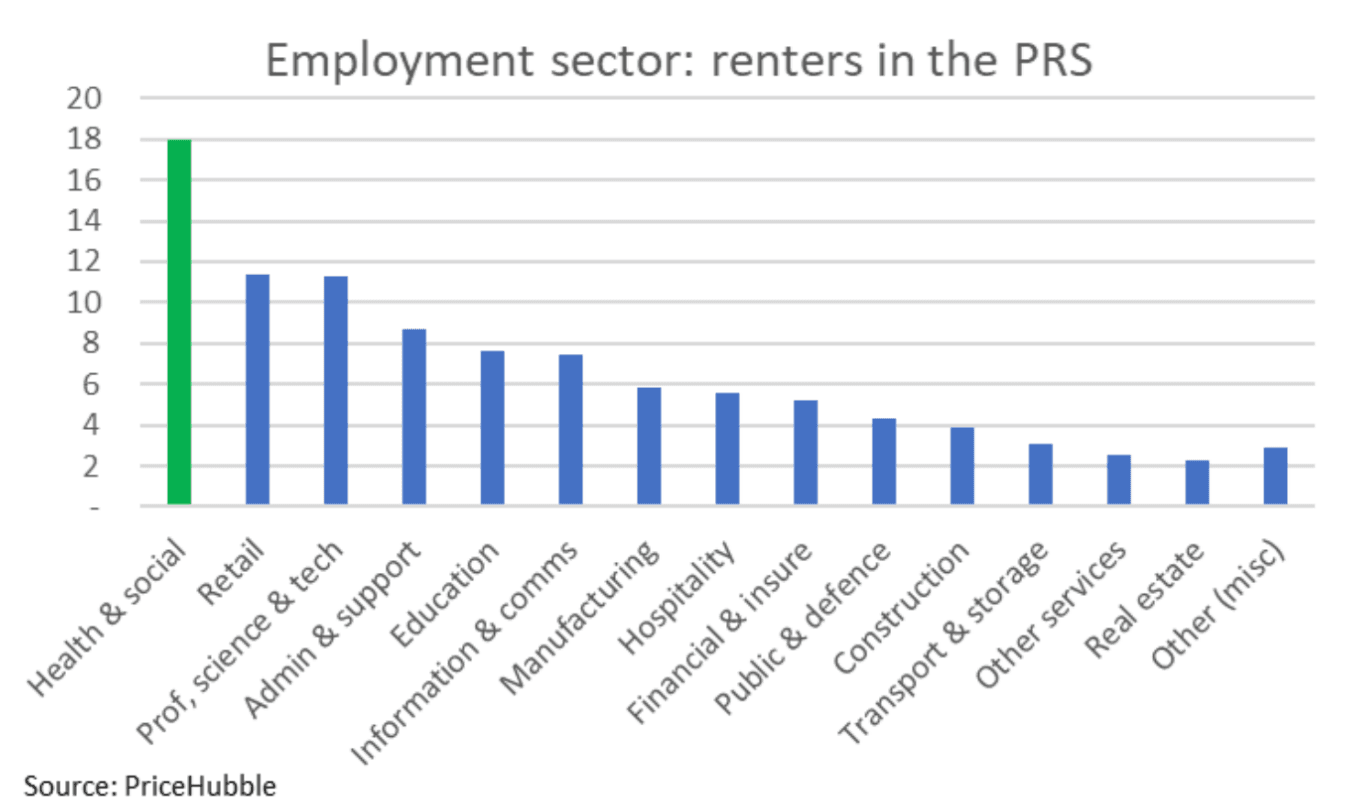
The scale alone is striking: approximately 18 per cent of working renters are employed in health and social care, making it the single largest employment category within the rental market. In real terms, this translates into more than one million NHS and social care workers living in the private rented sector.
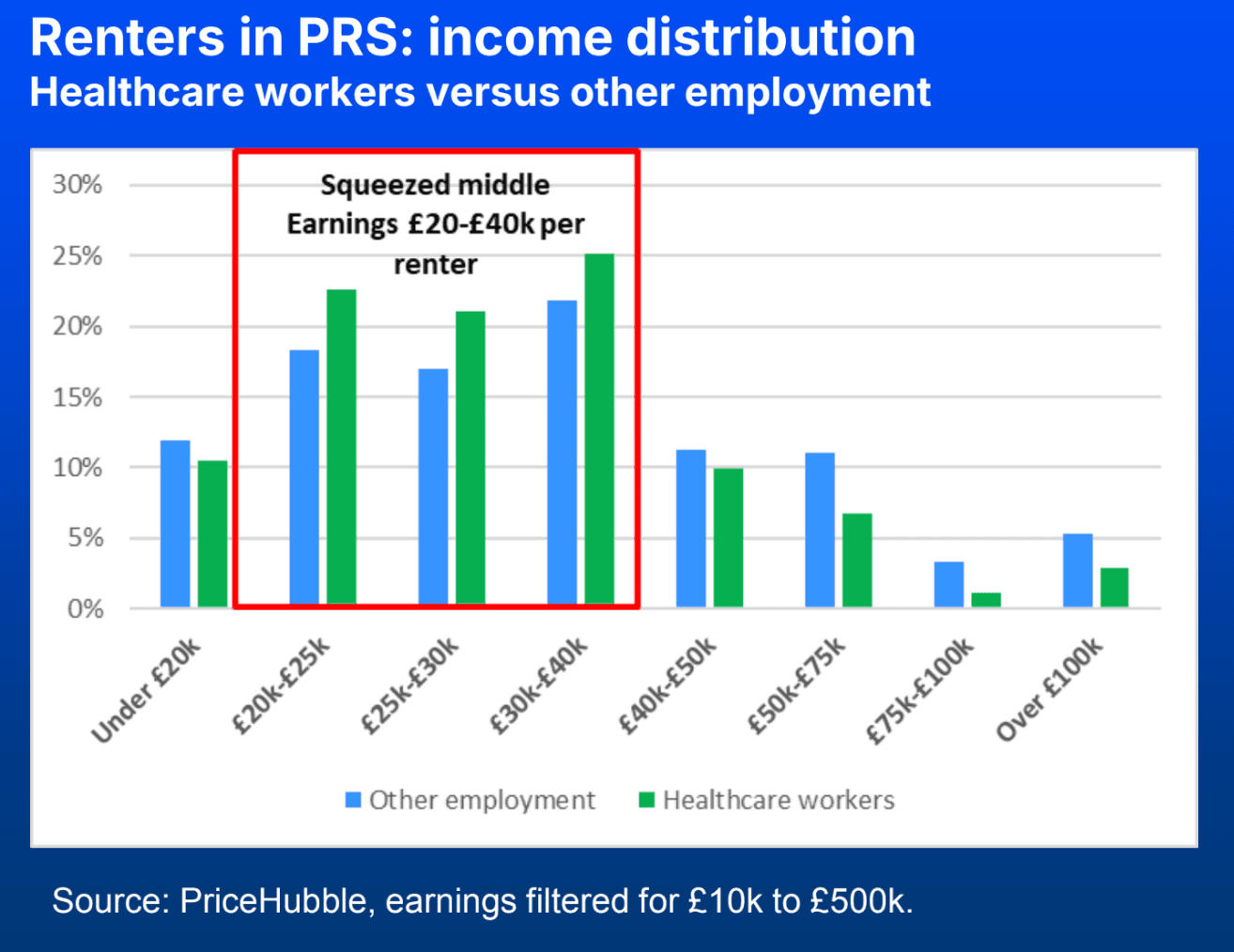
Crucially, many sit within what Middleton described as the “squeezed middle”: “Healthcare workers are more likely to fall into the £20,000 to £40,000 income bracket, where affordability pressures are particularly acute.”
In the South East, nearly half of healthcare renters spend more than 30 per cent of their gross income on rent, with one in five exceeding 40 per cent. These are not marginal deviations; they represent sustained financial strain.
Affordability constraints also shape geography. Research previously published by PriceHubble has shown that Healthcare workers tend to live closer to their place of work than other renters - unsurprising given the pattern of shift work. However, in higher-value locations, healthcare workers live significantly further from their workplaces. The same study also found that they compromise on the size and quality of rental homes in high-value locations. This clearly reflects economic necessity rather than preference – in other words, these are evidence of housing stress.
At the end of January, PriceHubble partnered with the Association for Rental Living (ARL) to host a discussion on a challenge that sits at the intersection of housing markets and public services: how the lack of affordable homes impacts the lives of key workers, particularly those employed in Health and Social Care.
The webinar brought together three complementary perspectives – market data, academic research, and delivery expertise – to explore what is now widely recognised as more than simply a housing problem.
Chaired by Sandra Jones, Managing Director at PriceHubble UK, the panel featured Dr Iqbal Hamiduddin, Associate Professor at UCL’s Bartlett School of Planning, Sarah Hordern, Non-Executive Director at the Oxford University Hospitals NHS Foundation Trust, CEO of Perspicio and Chair of the NHS Homes Alliance, and Julia Middleton, Real Estate Economist at PriceHubble.
Together, their contributions painted a consistent picture: housing affordability is critical to staff recruitment, retention and wellbeing.
The scale of rental dependence among healthcare workers
To set the scene, Julia Middleton shared metrics from PriceHubble’s achieved rents and renter demographics dataset, offering insights into the scale and characteristics of healthcare workers living in the private rental sector.
The scale alone is striking: approximately 18 per cent of working renters are employed in health and social care, making it the single largest employment category within the rental market. In real terms, this translates into more than one million NHS and social care workers living in the private rented sector.

Crucially, many sit within what Middleton described as the “squeezed middle”: “Healthcare workers are more likely to fall into the £20,000 to £40,000 income bracket, where affordability pressures are particularly acute.”
In the South East, nearly half of healthcare renters spend more than 30 per cent of their gross income on rent, with one in five exceeding 40 per cent. These are not marginal deviations; they represent sustained financial strain.

Affordability constraints also shape geography. Research previously published by PriceHubble has shown that Healthcare workers tend to live closer to their place of work than other renters - unsurprising given the pattern of shift work. However, in higher-value locations, healthcare workers live significantly further from their workplaces. The same study also found that they compromise on the size and quality of rental homes in high-value locations. This clearly reflects economic necessity rather than preference – in other words, these are evidence of housing stress.
At the end of January, PriceHubble partnered with the Association for Rental Living (ARL) to host a discussion on a challenge that sits at the intersection of housing markets and public services: how the lack of affordable homes impacts the lives of key workers, particularly those employed in Health and Social Care.
The webinar brought together three complementary perspectives – market data, academic research, and delivery expertise – to explore what is now widely recognised as more than simply a housing problem.
Chaired by Sandra Jones, Managing Director at PriceHubble UK, the panel featured Dr Iqbal Hamiduddin, Associate Professor at UCL’s Bartlett School of Planning, Sarah Hordern, Non-Executive Director at the Oxford University Hospitals NHS Foundation Trust, CEO of Perspicio and Chair of the NHS Homes Alliance, and Julia Middleton, Real Estate Economist at PriceHubble.
Together, their contributions painted a consistent picture: housing affordability is critical to staff recruitment, retention and wellbeing.
The scale of rental dependence among healthcare workers
To set the scene, Julia Middleton shared metrics from PriceHubble’s achieved rents and renter demographics dataset, offering insights into the scale and characteristics of healthcare workers living in the private rental sector.
The scale alone is striking: approximately 18 per cent of working renters are employed in health and social care, making it the single largest employment category within the rental market. In real terms, this translates into more than one million NHS and social care workers living in the private rented sector.

Crucially, many sit within what Middleton described as the “squeezed middle”: “Healthcare workers are more likely to fall into the £20,000 to £40,000 income bracket, where affordability pressures are particularly acute.”
In the South East, nearly half of healthcare renters spend more than 30 per cent of their gross income on rent, with one in five exceeding 40 per cent. These are not marginal deviations; they represent sustained financial strain.

Affordability constraints also shape geography. Research previously published by PriceHubble has shown that Healthcare workers tend to live closer to their place of work than other renters - unsurprising given the pattern of shift work. However, in higher-value locations, healthcare workers live significantly further from their workplaces. The same study also found that they compromise on the size and quality of rental homes in high-value locations. This clearly reflects economic necessity rather than preference – in other words, these are evidence of housing stress.
Research
Health workers living in private rental homes

Research
Health workers living in private rental homes

Looking behind the numbers: lived experience and workforce consequences
While market data demonstrates the existence of housing stress for Healthcare workers, it does not capture how those pressures are actually experienced. This is where Dr Iqbal Hamiduddin’s work adds depth.
Working directly with major London NHS Trusts, Hamiduddin and his team conducted employee surveys to examine the lived reality of staff navigating the housing market.
As he explained, Trusts had long suspected a link between housing costs and workforce instability. The research was designed to provide robust evidence, and what emerged was concerning: “Between the Trusts we studied, around 80 per cent of staff indicated they were considering leaving London within the next two years, citing housing pressures as a primary factor,” Iqbal Hamiduddin explained.
Staff turnover, already a persistent challenge for NHS employers, carries both operational and financial consequences. Iqbal Hamiduddin highlighted the scale of the impact: “The NHS estimates it costs around £12,000 to recruit and onboard a new nurse. When turnover rates reach 15 per cent annually, the cost implications quickly become significant.”
Beyond affordability, respondents also described widespread compromises in housing quality and suitability. Overcrowding, long commutes, and poor conditions were recurring themes. Many reported that housing difficulties had contributed to stress, fatigue, and even absence from work.
Perhaps most strikingly, a notable proportion of staff reported having experienced homelessness at some point during their NHS careers – a finding that challenges conventional assumptions about housing security among full-time healthcare professionals.
The research underscores an important point: affordability pressures are not abstract economic forces. They shape daily life, health, and employment decisions.
A challenge extending beyond London
Although London and the South East experience the most visible pressures, similar dynamics are emerging across the UK. Julia Middleton observed: “While the problem is most acute in London and the South East, we can see pockets of similar affordability challenges across many regional markets.”
Sarah Hordern reinforced this view with examples from outside the capital, pointing to locations where house price-to-earnings ratios, constrained supply, and short-term letting activity have intensified pressures on key workers.
The underlying issue is structural rather than regional: in many areas, wages for essential workers are increasingly misaligned with local housing costs.
The delivery dilemma: opportunity and constraint
If the need is so evident, why has delivery remained so limited?
For Sarah Hordern, the answer lies in the intersection of viability, public sector finance, and risk allocation. Higher development costs and interest rates have widened funding gaps, even where discounted land models are available. NHS Trusts’ landholdings offer potential, but capital expenditure rules and accounting frameworks complicate traditional delivery routes. “Why don’t Trusts just borrow and build? Because NHS capital budgets are already severely constrained,” Sarah Hordern explained.
The NHS Homes Alliance has been working with the government to explore partnership structures that can attract long-term private capital while remaining compliant with Treasury rules. Recent policy signals, including recognition of NHS homes within wider strategic planning, suggest growing momentum. “There is now a clearer understanding that private capital is not inherently problematic, but structures must be designed properly,” Sarah Hordern noted.
Housing as workforce infrastructure
A clear conclusion emerged from the discussion: affordable housing for healthcare workers is no longer a peripheral policy concern. It is workforce infrastructure. Housing costs influence not only where key workers live, but also whether they remain in high-pressure roles and high-cost regions. As affordability pressures persist, collaboration between healthcare providers, government, investors, and the rental living sector will be critical.
The evidence is there. The remaining question is how quickly it can be translated into delivery.
Looking behind the numbers: lived experience and workforce consequences
While market data demonstrates the existence of housing stress for Healthcare workers, it does not capture how those pressures are actually experienced. This is where Dr Iqbal Hamiduddin’s work adds depth.
Working directly with major London NHS Trusts, Hamiduddin and his team conducted employee surveys to examine the lived reality of staff navigating the housing market.
As he explained, Trusts had long suspected a link between housing costs and workforce instability. The research was designed to provide robust evidence, and what emerged was concerning: “Between the Trusts we studied, around 80 per cent of staff indicated they were considering leaving London within the next two years, citing housing pressures as a primary factor,” Iqbal Hamiduddin explained.
Staff turnover, already a persistent challenge for NHS employers, carries both operational and financial consequences. Iqbal Hamiduddin highlighted the scale of the impact: “The NHS estimates it costs around £12,000 to recruit and onboard a new nurse. When turnover rates reach 15 per cent annually, the cost implications quickly become significant.”
Beyond affordability, respondents also described widespread compromises in housing quality and suitability. Overcrowding, long commutes, and poor conditions were recurring themes. Many reported that housing difficulties had contributed to stress, fatigue, and even absence from work.
Perhaps most strikingly, a notable proportion of staff reported having experienced homelessness at some point during their NHS careers – a finding that challenges conventional assumptions about housing security among full-time healthcare professionals.
The research underscores an important point: affordability pressures are not abstract economic forces. They shape daily life, health, and employment decisions.
A challenge extending beyond London
Although London and the South East experience the most visible pressures, similar dynamics are emerging across the UK. Julia Middleton observed: “While the problem is most acute in London and the South East, we can see pockets of similar affordability challenges across many regional markets.”
Sarah Hordern reinforced this view with examples from outside the capital, pointing to locations where house price-to-earnings ratios, constrained supply, and short-term letting activity have intensified pressures on key workers.
The underlying issue is structural rather than regional: in many areas, wages for essential workers are increasingly misaligned with local housing costs.
The delivery dilemma: opportunity and constraint
If the need is so evident, why has delivery remained so limited?
For Sarah Hordern, the answer lies in the intersection of viability, public sector finance, and risk allocation. Higher development costs and interest rates have widened funding gaps, even where discounted land models are available. NHS Trusts’ landholdings offer potential, but capital expenditure rules and accounting frameworks complicate traditional delivery routes. “Why don’t Trusts just borrow and build? Because NHS capital budgets are already severely constrained,” Sarah Hordern explained.
The NHS Homes Alliance has been working with the government to explore partnership structures that can attract long-term private capital while remaining compliant with Treasury rules. Recent policy signals, including recognition of NHS homes within wider strategic planning, suggest growing momentum. “There is now a clearer understanding that private capital is not inherently problematic, but structures must be designed properly,” Sarah Hordern noted.
Housing as workforce infrastructure
A clear conclusion emerged from the discussion: affordable housing for healthcare workers is no longer a peripheral policy concern. It is workforce infrastructure. Housing costs influence not only where key workers live, but also whether they remain in high-pressure roles and high-cost regions. As affordability pressures persist, collaboration between healthcare providers, government, investors, and the rental living sector will be critical.
The evidence is there. The remaining question is how quickly it can be translated into delivery.
Looking behind the numbers: lived experience and workforce consequences
While market data demonstrates the existence of housing stress for Healthcare workers, it does not capture how those pressures are actually experienced. This is where Dr Iqbal Hamiduddin’s work adds depth.
Working directly with major London NHS Trusts, Hamiduddin and his team conducted employee surveys to examine the lived reality of staff navigating the housing market.
As he explained, Trusts had long suspected a link between housing costs and workforce instability. The research was designed to provide robust evidence, and what emerged was concerning: “Between the Trusts we studied, around 80 per cent of staff indicated they were considering leaving London within the next two years, citing housing pressures as a primary factor,” Iqbal Hamiduddin explained.
Staff turnover, already a persistent challenge for NHS employers, carries both operational and financial consequences. Iqbal Hamiduddin highlighted the scale of the impact: “The NHS estimates it costs around £12,000 to recruit and onboard a new nurse. When turnover rates reach 15 per cent annually, the cost implications quickly become significant.”
Beyond affordability, respondents also described widespread compromises in housing quality and suitability. Overcrowding, long commutes, and poor conditions were recurring themes. Many reported that housing difficulties had contributed to stress, fatigue, and even absence from work.
Perhaps most strikingly, a notable proportion of staff reported having experienced homelessness at some point during their NHS careers – a finding that challenges conventional assumptions about housing security among full-time healthcare professionals.
The research underscores an important point: affordability pressures are not abstract economic forces. They shape daily life, health, and employment decisions.
A challenge extending beyond London
Although London and the South East experience the most visible pressures, similar dynamics are emerging across the UK. Julia Middleton observed: “While the problem is most acute in London and the South East, we can see pockets of similar affordability challenges across many regional markets.”
Sarah Hordern reinforced this view with examples from outside the capital, pointing to locations where house price-to-earnings ratios, constrained supply, and short-term letting activity have intensified pressures on key workers.
The underlying issue is structural rather than regional: in many areas, wages for essential workers are increasingly misaligned with local housing costs.
The delivery dilemma: opportunity and constraint
If the need is so evident, why has delivery remained so limited?
For Sarah Hordern, the answer lies in the intersection of viability, public sector finance, and risk allocation. Higher development costs and interest rates have widened funding gaps, even where discounted land models are available. NHS Trusts’ landholdings offer potential, but capital expenditure rules and accounting frameworks complicate traditional delivery routes. “Why don’t Trusts just borrow and build? Because NHS capital budgets are already severely constrained,” Sarah Hordern explained.
The NHS Homes Alliance has been working with the government to explore partnership structures that can attract long-term private capital while remaining compliant with Treasury rules. Recent policy signals, including recognition of NHS homes within wider strategic planning, suggest growing momentum. “There is now a clearer understanding that private capital is not inherently problematic, but structures must be designed properly,” Sarah Hordern noted.
Housing as workforce infrastructure
A clear conclusion emerged from the discussion: affordable housing for healthcare workers is no longer a peripheral policy concern. It is workforce infrastructure. Housing costs influence not only where key workers live, but also whether they remain in high-pressure roles and high-cost regions. As affordability pressures persist, collaboration between healthcare providers, government, investors, and the rental living sector will be critical.
The evidence is there. The remaining question is how quickly it can be translated into delivery.
See also

News
Read more →

News
Read more →

News
Read more →
Request a demo
We will get back to you quickly.
We look forward to speaking with you.
Thank you!
We will get back to you within 24 business hours.

Thank you!
We will get back to you within 24 business hours.

Dataloft has now merged with PriceHubble.com
